Additive Manufactured Fixation Plates Better Match Patient's Jaw Bone
A combination of selective laser melting and NiTi material enabled the creation of plates matched to both the shape and stiffness of natural bone.
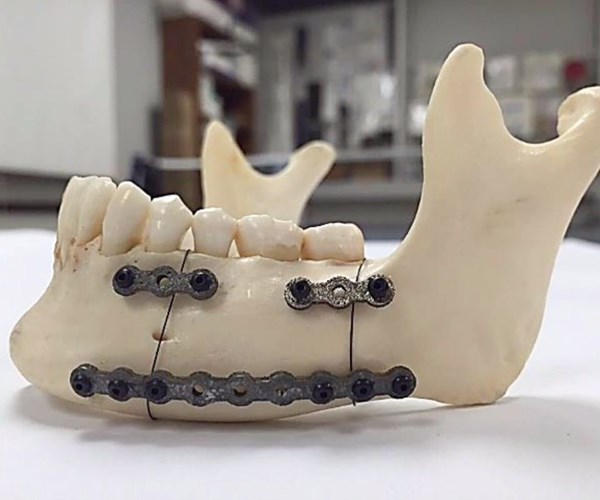
Researchers created porous fixation plates for reconstructive jaw surgery that precisely match the geometry as well as the stiffness of a natural jaw bone.
Traditionally, fixation plates—the implants used to support damaged bone as it heals—are manufactured to standard sizes, most commonly from Ti-6Al-4V. The surgeon chooses the plates closest to the patient's anatomy, and then bends them to fit in the operating room.
While effective, this method has several drawbacks. Working with standard sizes means that implants may not achieve a perfect fit with the patient, and the bending step adds time to reconstructive surgery. In addition, the Ti-6Al-4V material most frequently used is much stiffer than cortical bone, which can cause abnormal stress distribution and ultimately cause implants to fail.
In a study published by open-access journal Bioengineering, a team of researchers sought to create plates that would not only match the specific anatomy of the patient's bone, but also its stiffness. Using selective laser melting (SLM), the team 3D-printed custom fixation plates for mandible, or lower jaw, reconstruction surgery using NiTi. 3D printing the plates enabled the researchers to produce fixation plates that not only matched the shape of the cadaver mandible used in the study but also its stiffness. SLM enabled the creation of porous fixation plates with a cell pattern that allows for stiffness adjustment.
A CT scan of the mandible used in the study showed that the bone had a Young's modulus (the ratio of tensile stress in a material to strain) of 12 GPa. Dense samples made from NiTi with SLM had a Young's modulus of 37 GPa. To lower the stiffness of the material, researchers introduced porosity using identical unit cells. Adjusting the size of each cell enabled the team to adjust the porosity of the part as well as its stiffness.
To match the 12-GPa modulus of the natural bone, researchers determined that the fixation plates would require porosity of 45.7 percent and adjusted the unit cells to achieve this. The same stiffness modulus could have been achieved in the Ti-6Al-4V material, but this would have required a much higher porosity of 78.3 percent, and such an open structure can cause complications during manufacturing.
Applying this methodology could save time in the operating room and reduce the risk of complications from reconstructive surgery. Learn more about the benefits of 3D printing custom fixation plates and find a link to the full paper in this article from Additive Manufacturing, sister publication to Modern Machine Shop.
Related Content
-
Best Practices: Machining Difficult Materials
Cutting hardened steel, titanium and other difficult materials requires picking the right tools, eliminating spindle runout and relying on best practices to achieve tight part tolerances.
-
Modern Bar Feeds Bring New Life to Automatic Swiss Lathes
Cam-actuated Swiss lathes are still the fastest way to process many parts. By adding modern bar feeders, this shop has dramatically improved their utilization with the ability to work unattended, even in a lights-out environment.
-
SolidCAM Wants to Help Machine Shops Get into Additive Manufacturing
SolidCAM's partnership with Desktop Metal is aimed at making additive manufacturing more accessible to job shops and other manufacturers.

.jpg;width=70;height=70;mode=crop)













